 I daresay that melatonin is not the most exciting topic to be writing about in 2020 and you might wonder what I have to add. Well it’s a bit of an understatement to say I have an interest in women’s physiology.
I daresay that melatonin is not the most exciting topic to be writing about in 2020 and you might wonder what I have to add. Well it’s a bit of an understatement to say I have an interest in women’s physiology.
And for that reason, I want to look at three (relatively) less well known benefits of melatonin for women. Since my voice is shot from singing karaoke (no really) and I wrote the article first, there won’t be a video.
Table of Contents
Benefits of Melatonin for Women
Melatonin is a chemical produced in the brain that, among its other roles, regulates human sleep/wake cycles (see below). Certainly both women and men produce melatonin and it plays a similar if not identical role in both sexes. As well, there’s no doubt that it has potential benefits in both sexes.
So why am I writing an article specifically about the benefits of melatonin for women?
Well, there are a couple of reasons. The first is that, most recently, examining women’s physiology and sex based differences is kind of my thing of late.
There are often places where the specifics of women’s physiology suggests that women’s requirements or benefits from a given food or compound are different from that of men’s. One example I mentioned in The Women’s Book were cruciferous vegetables which may play a specific role in breast cancer prevention. Creatine is another that may have specific benefits for women.
And the same is true of melatonin. A little more specifically melatonin appears to have specific benefits in three different situations. The first of these is Pre-menstrual Syndrome (PMS)/Pre-Menstrual Dysphoric Disorder (PMDD). The second is Poly-Cystic Ovary Syndrome (PCOS). The third and final, and the only one that all women will experience, is the menopausal transition.
In all three of these situations, disturbances in the melatonin system may occur and be part of the problems that are seen. This gives melatonin supplementation the potential to have great potential benefit. I’ll come back to each below.
Melatonin Basics
I have to imagine that anyone reading this has at least heard of melatonin. I also suspect most have at least a general idea of what it does. Without getting into endless details that nobody cares about, here’s a short course on melatonin.
Melatonin is synthesized from serotonin and released from the pineal gland (the third eye, ommmm). Arguably it’s primary role is to regulate human sleep/wake and light/dark cycles. This gets into a bunch of technical details regarding circadian rhythms and the biological clock. Honestly, the details aren’t important here so I won’t get into them.
However, in addition to this primary role, melatonin does far more in the body. It has a direct effect on reproductive hormone rhythms for example. It does this by controlling GnRH (Gonadatrophic Releasing Hormone). This is the hormone that controls LH and FSH release, ultimately controlling estrogen and testosterone levels.
Melatonin also has an effect on body temperature, blood pressure, cardiovascular regulation and immune system function in addition to acting as an anti-oxidant and free radical scavenger.
In animal models, melatonin regulates energy expenditure and fat mass and there are melatonin receptors on fat cells, at least in animals. It also plays a role in regulating bone mass.
Note that animal research very often does not translate to humans in the least and I only mention this because the review paper I linked to did.
Related: How Many Calories Do I Burn Per Day?
The Rhythm of the Night
Under normal conditions melatonin shows a very distinct circadian (daily rhythm), going up at night and down in the morning.
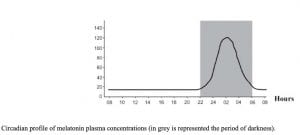
Melatonin levels are regulated by light entering the eye and this is the genesis of the idea of avoiding bright lights directly into the eye near bedtime as this will prevent melatonin going up as it normally would.
The blue light from electronic devices has this effect although other types of artificial lighting can as well. Many other aspects of sleep hygeine such as sleep masks, blackout curtains, etc. also derive from this idea. At one point it was thought that exposure of the skin to light could impact negatively on melatonin but this appears to be incorrect.
Low level of melatonin accompany a lot of different conditions including several psychiatric maladies. One of those is bipolar disorder. Perhaps the more commonly known one is depression where melatonin rhythms may be phase shifted.
By that I mean that the normal daily melatonin rhythm shown above could move to the left, with melatonin rising earlier and going down earlier than normal. This would cause someone to get sleepy early in the evening but wake up much earlier.
Alternately, it could shift to the right, going up later than normal and staying up later into the morning. This would make it difficult to fall asleep at night while leaving the person unable to become alert in the morning.
There’s a lot more to melatonin that I just don’t want to get into here. I will note that much of what I will discuss in terms of melatonin’s potential benefits is not related to sleep. In the case of PCOS and menopause, melatonin appears to provide far more benefits to women than just improving sleep.
Melatonin and PMS/PMDD
The first situation where there may be benefits of melatonin for women applies to pre-menopausal women with a “normal” menstrual cycle. Those situations are Pre-Menstrual Syndrome (PMS, also called Pre-Menstrual Tension) and the more severe Pre-Menstrual Dysphoric Disorder (PMDD).
A Primer on the Menstrual Cycle
As a brief introduction, after puberty, women experience a roughly monthly variation in their hormones and physiology. I say roughly monthly due to the fact that a “normal” menstrual cycle is defined as anything from 24-32 days even if we think of it as 28 days. Those changes affect nearly everything from appetite, insulin sensitivity, whether carbs or fats are preferentially used, etc.
Related: What Are the Differences Between Women and Men’s Physiology?
The cycle is divided into two phases: the follicular phase and the luteal phase with ovulation in the middle. The cycle, by convention, starts with the first day of bleeding and the follicular phase (where the follicle, containing the egg) lasting until ovulation when the follicle bursts and the egg is released.
After ovulation the luteal phase (named for the creation of the corpus luteum from the remains of the burst follicle) is formed. Across these 4 weeks a woman’s primary reproductive hormones, estrogen and progesterone vary in fascinating and complex ways. I’ve shown this below.
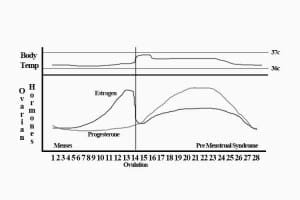
For the purposes of this section we are interested in the final “week” of the cycle, termed the late luteal phase. At this point both progesterone and estrogen are dropping and this is when many women will experience any number of negative effects. As indicated in the graphic, if it’s going to happen at all, this is when PMS will typically occur (note that there are other patterns in terms of when symptoms appear).
PMS and PMDD
The changes that occur during the late luteal phase are termed PMS or PMT (I think this is primarily a UK term). Depending on your source, PMS occurs in 30-40% of women. Cramps are the most common symptom, reported in 45-95% of women with 3-33% of women being physically incapacitated by them.
Other symptoms are common such as mood swings, depression, lack of motivation, etc. Women may suffer from headaches, joint or muscle ache, digestive problems, issues with coordination and many others. Exhaustion, irritability, anger, problems with concentration and mood swings are common as well.
Male coaches of women, keep this in mind when a woman comes to training in this phase of her cycle and seems less than fired up or agitated or depressed or what have you. It’s not laziness or craziness. It’s biology. You should take it into account and this can be a good time to plan an easy series of workout along with avoiding complex high-coordination exercises.
Blood sugar becomes unstable causing hunger or fatigue and a fall in dopamine allows prolactin to go up, causing breast tenderness. Serotonin is also dropping and this is a very likely cause of the mood changes that are occurring.
In any case, there is a more extreme version of PMS called PMDD. It only occurs in 5-10% of women but is often devastating to a woman’s well-being. All of the above occurs, often in more harsh versions and at the extremes, women with PMDD may experience suicidal ideation.
Anti-depressants are often used to treat severe PMDD (supporting a link to serotonin). As an interesting anecdote, my own nurse practitioner told me that in some cases, she will add an anti-depressant to the drug regimen for her patients during that week of their menstrual cycle.
Sleep and PMS/PMDD
And so far as this article is concerned, another issue of concern is that sleep patterns become impaired during this part of the cycle. To some degree, many women will experience sleep disturbances in the late luteal phase but at least some research finds that this is worse in PMS and the worst in PMDD.
In fact most of the work seems to be in women with PMDD. I still think it is relevant to women who “only” suffer from PMS, however.
I mentioned above that light going into the eyes is one part of what keeps melatonin from rising. As it turns out, light has an even greater impact on this in women with PMDD. This makes an even stronger case for women with severe PMS/PMDD to avoid electronic devices, etc. at night.
Women with PMDD also show a decreased response to the melatonin that is released. This causes her normal circadian rhythms to be disrupted and this may have to do with some of the mood changes that are seen (i.e. how good do you feel after a poor night’s sleep? Multiply that by 100).
All of this adds up to impaired melatonin rhythms contributing to both sleep disturbance which may have an add-on effect of increasing any mood changes.
Melatonin Supplementation for PMS/PMDD
Despite the research on this topic, it doesn’t appear that anyone has tested melatonin supplementation for treating either PMS or PMDD. Light box therapy, where someone sits in front of a light box in the morning has been examined and certainly this can be part of the approach. Sleep deprivation has also been used to try to “reset” the normal circadian rhythm. This doesn’t sound fun at all.
But nobody has yet to test melatonin supplementation directly. So consider what I’m about to write as speculative and nothing more. Direct research could very well come out saying I’m wrong and that’s ok.
But I do think that considering melatonin supplementation is worth considering here. It may not help but I don’t see how it can hurt. For basic sleep purposes, higher doses are not usually better. They can cause some freaky deaky dreams and often leave people feeling hung over.
Anywhere from 0.3 mg (300 mcg) to 1 mg would be a good place to start. It should be taken an hour before goal bedtime (i.e. take it at 9pm for a 10pm bedtime) as this will help to induce sleep. An additional consideration might be a time released form of melatonin which will keep melatonin levels up throughout the night to maintain sleep.
Again, this is very speculative and should be taken as nothing but that. Why nobody has tested this directly is simply beyond me.
Melatonin and PCOS
PCOS refers to Poly-Cystic Ovary Syndrome, one of the more common reproductive dysfunctions that occurs in women. PCOS is diagnosed by what is called the Rotterdam Criteria whereby a woman must have 2 or more of the following.
- Multiple cysts on the ovaries
- Hyperandrogenism (elevated levels of testosterone, DHEA and other compounds)
- Oligo-menorrhea or amenorrhea
Oligo-menorrhea refers to infrequent menstrual cycles occurring every 35-90 days and amenorrhea refers to the absence of a menstrual cycle (technically less than 3 cycles in a year).
It’s important to realize that PCOS encompasses a number of conditions (and there is some push to consider them distinctly). Because when you consider 3 criteria with 2 (or 3) meeting the diagnoses, you end up with 4 possible situations with the severity decreasing from Type I to Type IV.

It might seem odd that a woman can have Poly-Cystic Ovary Syndrome without having multiple cysts on the ovaries but I don’t make up the rules. Mostly I think this reflects the realization that PCOS is not a single condition but rather a cluster of different metabolic dysfunctions.
It’s equally important to realize that a lot of the “problems” that occur in PCOS are due to the hyperandrogenism which is not present in all subtypes. That said, 3 of 4 Subtypes (1-3) have hyperandrogenism as a symptom and it is found in roughly 60% of all PCOS cases.
It is this hyperandrogenism that causes many of the problems that occur in PCOS including carrying more bodyfat around the midsection. It is also associated with the commonly seen insulin resistance that occurs. Finally, it is strongly involved in the menstrual cycle dysfunction that is seen.
At the same time, the elevated androgen levels that occur can benefit female athletes. Women with PCOS are frequently found at the highest levels of sport including the Olympics. Their elevated testosterone levels (often double that of non PCOS women) lead to increased muscle mass, strength and denser bones.
PCOS women may have a higher VO2 max (a marker of aerobic performance) an improved ability to recover and adapt to training more effectively, etc. Some have even asked if PCOS should be considered a “doping” condition, similar to that of a woman using anabolic steroids.
I bring this up as some of the effects of melatonin discussed below work by reducing androgen levels. For a woman with PCOS looking to improve her health and/or fertility this should be seen as a good thing. However, for female athletes, the effect of melatonin can be seen as a negative. Reducing their testosterone levels will, if anything, take away some of their inherent hormonal advantages in a sporting context.
Melatonin Levels and Effects in PCOS
While sleep disturbances are common in PCOS this is thought to be related to factors other than melatonin per se. One research group found that high nighttime melatonin was associated with poor sleep quality and increased oxidative stress. But it’s not clear if the increased melatonin is the cause of the poor sleep or rather a symptom of something else (I suspect the latter).
Of some interest, higher melatonin is also associated with higher testosterone levels. Specifically melatonin levels were doubled in PCOS women and this was associated with a 72% higher testosterone level. I am not saying that the melatonin caused the elevation, only that they were correlated with one another. It’s entirely possible that high testosterone increases melatonin as the opposite.
Related to this, another group found that PCOS women have a lower day-night difference in melatonin levels. Recall that melatonin is supposed to go way up at night and then drop back down but this appears to not happen in PCOS women. This suggests that the normal melatonin rhythm has been altered.
Melatonin Supplementation in PCOS
Irrespective of the complex interactions between melatonin and various aspects of PCOS, there is some evidence that melatonin supplementation can be beneficial. Certainly this seems contradictory given the already elevated levels that are seen. More likely is that supplementation helps to normalize the altered melatonin rhythm.
In a 2017 pilot study, women with PCOS were given 2 mg/day of melatonin for 6 months. Over that time period, there was a decrease in androgen levels along with a slight decrease in BMI (oddly waist circumference did not change). All of the women were oligo-menorrheic to begin with and an amazing 95% of them saw an improvement in their menstrual cycle function.
In a 2019 study, women with PCOS were given 5 mg of melatonin 2X/day which is an admittedly odd dosing schedule. Overall the women saw a decrease in hirsutism (increased body hair, which is common in PCOS), total testosterone, and CRP while increasing levels of the body’s own anti-oxidants.
A recent review, examining 15 human studies (and 7 animal studies) concluded that melatonin supplementation in PCOS can enhance the quality of the egg (and embryo in the case of pregnancy), reduce obesity and inflammation and help to reduce the insulin resistance so common to PCOS.
The human doses varied from 1-3 mg although several of them combined the melatonin with other compounds (myo-insitol in one, metformin in another) which isn’t terribly good design since you don’t know if it’s one or the other compounds or the combination that is effective.
Regardless, it appears that melatonin supplementation, perhaps with other supplements (discussed in detail in The Women’s Book Vol 1) can improve many of the negatives that accompany PCOS. Given that one mechanism by which melatonin works is reducing androgen levels, this may not be a good strategy for competitive female athletes with PCOS.
Melatonin and Menopause
The final situation where there may be specific benefits of melatonin for women is during menopause. Of all three situations I’ve discussed, this is the one that all women will experience.
Menopause refers to the time in a woman’s life where her reproductive organs essentially cease functioning. This happens over time as women move through peri-menopause (literally near menopause) into menopause itself. During this time ovulation will come more infrequently until it stops completely at which point estrogen and progesterone will not be produced as during the menstrual cycle.
A staggering number of changes occur after menopause and the number of possible symptoms associated with it is enormous. Many of these are related to dropping estrogen levels, including an increase in bodyfat and bodyweight, a shift to a more central fat pattern, increased heart disease risk, bone loss and many others. Hormone replacement therapy helps to ameliorate much of this although similar effects can be had with non-hormonal supplements. I discuss this in detail in The Women’s Book Volume 1.
Menopause, Sleep and Melatonin
Anyone that has spent time around their grandparents has probably observed that their sleep patterns can get a little bit strange. I vividly remember my own grandmother going to bed every night at 8pm but being up at 4:30am doing stuff around the house. It made sleeping in the basement during Christmas holidays very interesting as I heard her walking around. But I digress.
As readers might expect at this point in the article, sleep does worsen with age and this is certainly true for women during menopause. This may include difficulty falling asleep, waking up in the middle of the night or early in the morning. Given the role of melatonin in controlling reproductive hormones, it’s even been suggested that changes in melatonin may be playing a direct role in menopause.
As with sleep issues in PCOS, it’s important to realize these sleep issues aren’t automatically or solely related to melatonin levels (they aren’t universal either). Menopausal women often experience a number of negative effects (i.e. hot flashes) that may contribute to sleep issues.
That said, melatonin levels do decrease with age and reach a minimum at menopause and it assuredly plays at least some role. At least some research has found that melatonin supplementation can improve sleep in post menopausal women.
However, the potential benefits of melatonin for post-menopausal women goes far beyond simply improving sleep. In many ways, it seems like its effects are almost too good to be true.
Melatonin Supplementation in Menopause
As I mentioned above, there are a staggering number of negative effects that occur during menopause/the menopausal transition (also called the climacteric).
In one study, 3mg of melatonin for 3 months led to a reduction in an overall climacteric score. Basically, the number and/or severity of menopausal symptoms was decreased. In another, 3 mg of melatonin for 3-6 months led to an increase in thyroid hormone, improved GnRH levels and a general improvement in mood and reduction in depression (also common after menopause). That alone would make melatonin worth considering.
But wait, there’s more.
Melatonin may also improve body composition. In one study, women were given 1-3 mg of melatonin per night for a year. The paper reported that they lost 6.9% fat while increasing their lean body mass by 5.2%. Frustratingly, neither initial nor final body composition data was provided and nowhere did I find what actual magnitude of change those percentages represented in terms of pounds or kilograms. I detest when studies do this because big percentage changes often mean irrelevant real world changes.
Irrespective of that there’s an important final reason for women going through menopause to consider melatonin and that is bone health. At menopause, women’s loss of bone mineral density (BMD) accelerates, especially if they forego hormone replacement therapy (HRT). Depending on a number of factors, this can eventually predispose women to osteopenia or full-blown osteoporosis.
Osteopenia is defined as having BMD one standard deviation below the normal value for a given age. Osteoporosis is defined as a BMD two standard deviations below the normal value for a given age.
And it appears that melatonin can help. Three studies have been done on the topic that I am aware of. The first gave 14 menopausal women 3 mg of melatonin for 6 months. While there was no measured change in BMD, the ratio of bone formation to bone breakdown was improved. This is a good sign but ultimately not that convincing.
Two other studies found far better results. In the first, women with osteopenia were given 1 or 3 mg of melatonin along with calcium and Vitamin D for a full year. The 1 mg group increase BMD in the femoral neck (in the leg) by 0.5% with no change in spinal BMD. In contrast, the 3 mg group improved femoral neck BMD by 2.3% and spinal BMD by 3.6%.
In the second, women were given 5 mg of melatonin along with strontium, Vitamin D and Vitamin K2 for one year. In addition to other benefits such as reduce inflammation, the women saw a 4.3% increase in spine BMD and a 2.4% increase in the femoral neck.
Certainly in the two latter studies other nutrients important to bone health were given. But that doesn’t change the magnitude of the results. I have to wonder what would have been accomplished if heavy weight training, known to improve BMD even after menopause, had been included.
Benefits of Melatonin for Women Redux
So let me sum up quickly. In addition to its other potential benefits, it seems like melatonin has some specific benefits to women in at least three situations.
The first is for women who suffer from PMS/PMDD. Here, it’s primarily role is in helping to regulate sleep during the fourth week of the menstrual cycle. Fairly low doses seem to be needed here and I’d tentatively recommend 0.3-1 mg an hour before bedtime. An additional 1 mg of time released melatonin might be worth trying to help maintain sleep through the night.
In PCOS, there seem to be impaired melatonin rhythms where melatonin is higher in the evening but doesn’t go down as much as it should during the day. Several studies doses ranging from 1-5 mg have shown fairly major benefits including decreased BMI, improve hormone levels, improved fertility along with decreased body hair and testosterone levels (let me note again that these effects would be a negative for female athletes with PCOS).
Finally there are enormous potential benefits to melatonin during menopause. In addition to any sleep promoting effects, melatonin at doses of 1-5 mg per night has the potential to decrease overall negative symptoms of menopause along with improving body composition and increasing BMD (if other nutrienst are present).
It’s honestly looking to me like melatonin is shaping up to be another one of those “seems too good to be true” types of supplements. If I hadn’t read the research I linked to above, I’m not sure I would have believed the potential benefits. I felt the same way about fish oils. If I had seen a list of the effects without having read the research, I wouldn’t have believed them.
I’d mention that melatonin is the tip of the iceberg for dietary supplements that can help women address the issues inherent to PMS/PMDD, PCOS or menopause. I discuss them all in my Women’s Book Volume 1.
No, I don’t know when Volume 2 will be done.

Facebook Comments