Every so often the idea that carrots or some other fairly innocuous food is bad due to a high Glycemic Index (GI) comes through the fitness industry. I can recall seeing it 3-4 times over my career. Invariably this is an overreaction due to not really understanding what the Glycemic Index really represents. So to help clear it up I want to look at the GI concept in some detail along with a related concept called the Glycemic Load (GL). And while I’ve done a full guide to dietary carbohydrates before, I want to start with a quick precis on how carbs are classified in the diet.
Table of Contents
Classifying Carbohydrates
How to classify different carbohydrates in the human has been a topic for decades if not the better part of a century (I’m sure it goes back further than this but I’m not sugar historian) and to make this article make sense, I want to blather about the different types of carbohydrates.
Fiber
Let me start with fiber. Composed of a variety of different compounds that I will not name but you can look at here if you really want fiber can be roughly divided into two categories. The first are insoluble fibers. These don’t mix in water, can’t be digested by humans and basically act as a broom in the gut.
The other are the soluble fibers, they mix in water (guar gum is a popular supplement, add it to water and wait and it will turn into a brick) and are digested in the body. However, unlike other carbohydrates these are fermented in the gut by bacteria into short-chain fatty acids (SCFA). These have a number of profound health benefits and actually provide 1.5-2 cal to the body (although it’s not considered carbohydrate grams of calories).
Digestible Carbohydrate
Digestible carbohydrates are all built from the same basic building blocks which are the monosaccharides (‘mono’ = one and ‘saccharide’ = sugar) which are glucose or blood sugar, fructose or fruit sugar, and galactose (not to be confused with Galactus, eater of worlds).
Quick note: all sugars end in -ose. There are other monosaccharides, ribose (which was once sold as a sports supplement) is one but they aren’t that important in the diet.
These single sugars bond into two molecule compounds called disaccharides (‘di’ = two) and the primary ones are sucrose (table sugar) which is glucose+fructose, lactose (milk sugar) which is glucose + galactose, and maltose (used to make beer) which is glucose + glucose.
Quick note: high-fructose corn syrup or HFCS is a man-made sugar that I’ve written about before. Despite it’s name, it’s almost identical to sucrose in composition and works the same in the body. While blamed for all modern ills by some including obesity, diabetes, the economy and the dissolution of the nuclear family (Ok, not really), this is alarmist nonsense. HFCS is found to a great degree in sugary sodas and, if there is a problem with it, it’s that most liquids don’t make people full and many are overconsuming a crap-load of CALORIES by drinking these drinks.
And while it’s popular to blame HFCS/sugary sodas for everything right now, let’s face facts: people who are drinking a Super Mega Giganto Big Gulp of coke have a diet and lifestyle that is total crap. HFCS isn’t helping but it’s the least of the problems here: simply, the HFCS per se is irrelevant to the calorie load.
And yes, I’m aware of the fructose overfeeding studies but here’s the thing: HFCS is not pure fructose to begin with and most of these studies use impossible amounts of the stuff . One used 300 grams of pure fructose which would be 600 grams of HFCS and yeah 2400 calories of straight sugar is probably unhealthy That much fructose/HFCS is irrelevant to normal human consumption pattersn.
There are some intermediate chain lengths that aren’t that important in the diet overall and once you get past the mono- and di-saccharides you are generally looking at longer chains of straight glucose. In the body these long chains of glucose are called glycogen and are found in both the liver and muscle. In the diet they are called starch or simply complex carbohydrates.
There are some other weird carbohydrates that come up sometimes. Maltodextrins are medium chains of glucose that are found in some specialty sports supplements as are amylopectins. There are also what are called resistant starches, carbohydrates modified to be resistant to digestion that may have health and metabolic benefits. These are being found in more and more foods and are good for dieting since you can eat the same volume of food but at least some of the starch won’t be digested or absorbed.
Digestion and Absorption of Carbohydrates
Focusing on the digestible carbohydrates, let me briefly talk about their digestion and absorption in the gut since this is important background for the actual stuff about Glycemic Index and Glycemic Load. A little bit of carbohydrate digestion actually starts in the mouth, via an enzyme called alpha-amylase (note: all enzymes end in -ase and there are lipases which digest fat and proteases that digest protein).
You can test this if you want, put a small piece of bread in your mouth (or hell a big piece, I’m not here to judge you) and chew on it without swallowing. You’ll start to get a sweet sensation in your mouth from the breakdown of the starch into individual molecules of glucose.
After what little digestion occurs in the mouth the food moves to the stomach where it is mechanically churned and broken down and acted on by more digestive enzymes. And here’s the key to this: only single sugars can be absorbed across the gut. You can’t absorb sucrose, you can’t absorb lactose, you can’t absorb starch directly. You can only absorb glucose, fructose and galactose and that’s all that hits the portal vein on the way to the liver.
So sucrose is broken down to one glucose and one fructose, lactose is broken down into one glucose and one galactose and longer chains of glucose such as maltodextrins, amylopectins or starch are broken down bond by bond into single molecules of glucose. And that’s all that hits the bloodstream.
After absorption, sugars are metabolized differently. Glucose generally moves straight through the liver out into the bloodstream where it is used for energy directly (most tissues can use glucose for energy and it is preferred when it is available) while fructose and galactose have to be metabolized in the liver first.
Fructose can be converted into glucose and either stored as liver glycogen or released into the bloodstream as glucose. It can also be converted to lactate which is used by other tissues; in large amounts (more than about 50 grams per day, fructose can be converted into fatty acids in the liver).
Note that fructose never gets into the main circulation in any significant degree and I mention that as some fear tactic bs has been based on fructose INFUSION but this has no relevance to eating food. Galactose is metabolized similarly to fructose but unless someone’s diet contains a shedload of milk, it’s really not worth worrying about.
Practically what this means is that regardless of what dietary carbohydrate is eaten, only glucose and fructose (and fine, galactose) make it out of the gut and only glucose ever makes it past the liver.
In one sense, this makes all dietary carbohydrates identical: one way or another they all end up as glucose in the bloodstream. Whether you eat pure glucose (don’t do this, it’s disgusting), maltodextrins or starch, it all ends up as glucose in the bloodstream at the end of the day. Even fructose eventually hits the bloodstream as glucose.
Which raises the question of what makes one dietary carbohydrate different from another.
The short answer is their speed of digestion.
So what’s the long answer?
Diabetes Treatment: Part 1
In the early days of nutrition, here I am talking about the first half and maybe a little bit later in the 20th century, it was generally thought that sugars were more or less “bad” and starches/complex carbohydrates were “good”.
At least some of this was based on nothing more than the foods that each were found in were generally thought to be “healthy” or “unhealthy”. Sugar bad, complex carbohydrates good, ook ook. It’s worth noting that fruits contain simple sugars and, especially at the time, few would have considered those unhealthy. That type of extremist stance would come later (thanks, Parillo).
But of more relevance to this piece was interest in treating diabetes. There are two kinds of diabetes which are Type I and Type II. Type I diabetes is a genetic condition where the pancreas doesn’t produce insulin. Until insulin was synthesized in the early 20th century, it was untreatable. Now it is but requires regular insulin injections.
Type II diabetes certainly has a genetic aspect but is mostly lifestyle related. Obesity, inactivity and a bad diet all contribute and the basic gist of it is that the body becomes insulin resistant which simply means that the hormone insulin can’t do it’s job in terms of storing nutrients in tissue like skeletal muscle and fat cells. A lot happens here but a common effect is increased blood glucose levels; since insulin can’t push glucose into muscle or fat cells, it hangs around in the bloodstream and this eventually causes damage to the body.
Note: Type II diabetes used to be called Adult Onset Diabetes since it was almost exclusively seen in adults (Type I, as a genetic condition shows up very early in life). This is no longer the case as more and more children are developing the condition due to increasing levels of obesity and inactivity. So now it’s just Type II diabetes. There is also the Metabolic Syndrome (formerly Syndrome X) which consists of a whole bunch of different metabolic dysregulations that tend to occur together.
The Glycemic Index: Part 1
For a lot of years, like most of the 20th century, the basic advice for diabetics was to limit simple sugars and consume primarily complex carbohydrates as it was assumed that simpler sugars, since they digested faster, would impact on blood sugar worse than more complex carbs. But as is commonly the case, the assumption wasn’t quite correct although it would be a while until it was formally tested and this was determined.
So far as I can tell, the first study to look at this more systematically was in 1981 when the first paper on the Glycemic Index (GI) was published. Originally, subjects were fed 50 grams of pure glucose on an empty stomach after an overnight fast and the blood glucose response was measured. More specifically the Area Under the Curve or AUC of blood glucose over 2 hours was measured. So imagine that the food is eaten and blood glucose is measured. It will go up over some time frame, maybe stay high and then come back to normal. This forms a curve. The total area under that curve is the AUC. Here’s kind of what it looks like and if you took high school calculus, you may remember how some of this works.
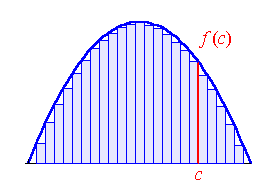 This value of AUC is arbitrarily defined as 100 and I need to make it very clear that the 100 doesn’t actually mean anything. It’s not the actual area under the curve or anything to do with blood glucose. It’s just an arbitrary reference value. You could define it as 1, 473 or Bob and means just as much. And that’s because GI is just a relative/comparative scale where the AUC of a given food is compared to the test food.
This value of AUC is arbitrarily defined as 100 and I need to make it very clear that the 100 doesn’t actually mean anything. It’s not the actual area under the curve or anything to do with blood glucose. It’s just an arbitrary reference value. You could define it as 1, 473 or Bob and means just as much. And that’s because GI is just a relative/comparative scale where the AUC of a given food is compared to the test food.
So after feeding them the 50 grams of pure glucose, at some later point, you feed them the equivalent of 50 grams of digestible carbohydrate of some other food and measure that AUC as well. Then you compare the two. If the second food has an AUC that is 70% of the reference food, the GI is 70. If that second food has an AUC that is 110% of the reference food, the GI is 110. Beating a dead horse (what is the GI on horse meat), it’s just a relative value.
If you had called the AUC Bob the two other foods would be 70% Bob and 110% Bob. Relative values.
The methodology of the GI changed a bit later (I honestly don’t know when). It was felt that 50 grams of glucose didn’t represent a real world situation and the reference food was changed to 50 grams of digestible carbohydrate from white bread (tho I think some studies still use glucose as a test food).
Everything else was the same, subjects were fed white bread and AUC was measured. Then they were fed another food, AUC was determined and the values were compared. There are charts online that show the two different sets of values and the relative positions of the foods don’t change although the actual numbers do. It’s just that glucose is now higher then 100 since white bread is the standard.
The Glycemic Index: Part 2
And even after the first study/studies were done, some interesting observations were made. One, that has recently become a big deal for some reason is that there was pretty large variability between people and that might point out that it’s fairly unreliable (it might also explain some of the divergent study results that I’ll mention).
Clearly you can’t define a diet by GI if two different people have completely different blood glucose responses. But that’s neither here nor there. Of more importance was that the old assumptions about simple and complex carbohydrates didn’t turn out to be completely correct.
Some complex carbohydrates generated a pretty large blood glucose response while some simple sugars didn’t. Fructose was a good example and had a very low GI which made it attractive as a sweetener. Pure fructose was super popular in the health freak community for a while which is about the only time that pure fructose feeding studies might have meant a damn. But most people can’t handle a large amount of it in pure form without stomach upset.
But the low GI of fructose was due to fructose first needing to be metabolized in the liver, converted to glucose/glycogen and then released into the bloodstream as glucose. This takes time and that gave fructose a low GI score.
Glucose was high of course since it gets right into the bloodstream and was the original test value. Sucrose (which recall is a glucose bound to a fructose) was halfway between fructose and glucose as you might expect. This is an important point I’ll come back to: when you add carbs together, the resulting GI ends up being the weighted average (more or less) of the two.
But it was even weirder than that as frequently complex carbohydrates had higher GI’s than sucrose. For example, white potatoes turn out to have a HIGHER GI than table sugar while sweet potatoes are about the same. Let that roll around in your head for a second, a baked potato (which most would assume is healthier due to it’s complex nature) generates a higher blood sugar response than straight up table sugar.
All three are much higher than fructose. On at least one scale, potatoes come in with a GI of about 80 depending on how it is cooked, sweet potatoes are about 63 with table sugar at 65 and fructose at 15. Even brown rice has a GI of 68. I think you get the idea.
There were at least some generalities. Generally more complex carbs, especially if they were high in fiber tended to have a lower GI than more refined and/or low fiber carbs. Beans are all pretty low on the GI scale but they contain fiber and protein. So is fruit, probably due to the small amount of fiber and the fructose content. Ice cream actually had a very low GI due to the fat content (see below). Looking only at the GI, ice cream is an excellent food for diabetics (hmm….)
The above would lead to a complete shift in diabetic meal planning from complex and simple carbs to diets based around GI. Since the largest issue with diabetics is keeping blood glucose stable and controlled, using GI was deemed to be more effective.
By eating low GI foods you lowered blood glucose and certainly some studies showed improved values (note that actual weight/fat loss always improves diabetic issues almost regardless of how you do it). The problem was that GI is not easy to use (one researcher described it as deceptively complex). There are also a significant number of issues with it beyond that I’ll discuss in the next part of the series.
Glycemic Index for Weight Loss
As you might imagine, the development of the GI was examined for other populations. One was weight loss and at least some studies showed that low GI foods were more filling than higher GI foods and generated better fat loss. This was questionable and the study results were about half and half. Not everyone agrees. I think that part of the problem is invariably that other nutrients are being impacted by high and low GI diets. Fiber intake usually varies and we know that fiber is filling. So does protein and protein is the most filling nutrient of all.
If a low GI diet causes someone to eat more protein, it will work better to keep them full due to the higher protein. It’s hard to do exact comparisons of low and high GI without other stuff changing. To take this into account, exactly one paper tried to determine a Satiety Index (how filling a given food is) all the way back in 1995 but for whatever reason, nobody ever bothered to follow up on it.
I think it was due to enormous individual variability but I wouldn’t swear to that. And, of course, GI has the same issues here as elsewhere in terms of being difficult to use. Certainly a diet telling someone to eat more beans, fruits and whatever amounts to low GI carbs is not a bad thing but that’s just focusing on things like fiber, slower digestion, etc. Trying to use GI in the real world is just a pain.
Glycemic Index and Athletes
And then of course there were athletes. Certainly for some performance sports, variations in GI can matter under certain circumstances. There has been some interest for example in low vs. high GI foods before competition (usually endurance type events) where it’s often recommended to consume low GI foods. Some very early work suggested that blood sugar might drop with carbs right before competition but this is individual and fairly irrelevant. Low GI foods to give a more even blood sugar response.
In one sense this is good in that it pushes carbohydrate oxidation during exercise (carbs are more efficient than fat). But it also inhibits fat mobilization and this could be problematic for long-events due to the benefit of using fat for fuel to spare muscle glycogen. So it’s a mixed bag and depends on the type of competition.
For a time-trial (a fixed distance event raced at maximum effort) using carbs is superior. For a 4 hour cycling race that will do a lot of time at lower intensities, sparing glycogen is paramount. There is also the issue of low GI foods potentially causing stomach upset because they digest more slowly. This tends to be of more relevance for running due to the movement in the stomach (it’s actually called “joggling”) and less so for other sports.
During workout has the same basic set of issues although it’s more common to consume more rapidly digesting carbohydrates under these conditions to avoid stomach upset.
For glycogen resynthesis following training or competition, GI may matter. This is especially true when rapid glycogen resynthesis is needed. Here higher GI foods consumed in small amounts frequently for the first 3-4 hours work better than lower GI foods. But even this is only important when an athlete has two intensive training bouts within 6-8 hours of one another.
So long as an athlete either a) does not fully deplete glycogen and b) has 20-24 hours between workouts for the same muscle groups, the rate of glycogen resynthesis is irrelevant (at the slowest rates you can hit 100% in about 20 hours) and low and high GI both work identically.
And then there are physique athletes. I don’t know if they were the first to get hung up on the GI but certainly they got very hung up on it and certain foods (such as carrots, often high GI) were flat out put on the never eat list (I’ll discuss why this is nonsensical in the next part).
First it’s important to realize that training status modulates GI, the more well (at least aerobically) trained you are, the lower the GI for any food. Training improves insulin sensitivity across the board (as does being lean generally) and since insulin response to food is part of this, GI goes down.
Certainly lower GI foods can be more filling (again, fiber, protein, etc.) which is nice but the assumption here usually had to do with GI and the insulin response to foods (insulin was bad since it inhibited fat mobilization and/or increased fat storage). The assumption was that lower GI meant a lower insulin response; as I’ll discuss in the next part that’s actually not always (or possibly even generally true). But there are issues with this.
Even basal levels of insulin after an overnight fast inhibit lipolysis by about 50% (Type I diabetics who let insulin fall too low get enormous fatty acid release) and this is a safety valve to keep the body from flooding the bloodstream with fatty acids which can cause problems. Raising insulin above basal fasting (basically when you eat anything) inhibit lipolysis pretty extremely/almost completely and it doesn’t look like GI really impacts on fuel partitioning, fat gain, or fat loss to any significant degree.
Make no mistake work here is usually done on overweight people and it’s entirely possible that a very lean individual dieting to the extremes is in a different situation. One adaptation to dieting is a huge improvement in insulin sensitivity and this is clearly to limit further fat mobilization so keeping insulin lower during extreme diets does make some logical sense. But even correlating that with the GI per se is problematic.
Problems with the Glycemix Index
While the GI concept made a lot of sense in that carbohydrates would digest and impact on blood glucose differently, there were a lot of problems with the method. Perhaps the largest was the most obvious: feeding someone 50 grams of digestible carbohydrate after an overnight fast isn’t really that relevant to how people eat in the real world in a number of ways.
Problem 1: Only One Meal is Eaten After Fasting
Yes, fine, breakfast by definition occurs after an overnight fast but are measurements made at that single time point indicative of the rest of the day? It turns out that the answer is no.And it was found early on that there was a second meal effect, that how the body responded to the next meal of the day could be profoundly different. In one study, a low glycemic dinner changed the glycemic response to breakfast on the next day.
Things like insulin sensitivity may change during the day, a previous meal may still be digesting and there were clearly residual hormonal effects from the first meal that impacted how the body responded at the second meal (I’m not getting into this but there are a huge number of hormones, incretins, etc. released when people eat that impact on all of this).
I mentioned above that training impacts on insulin sensitivity and I’d mention in passing that the idea that insulin sensitivity is always highest or lowest at some point in the day is always measured in diabetics. If you train at night, your insulin sensitivity is high no matter what a non-training diabetic with god knows what else is going on may be.
Problem 2: Few Eat a Single Carbohydrate Source
A second major issue is that GI is invariably tested with a single source of carbohydrates, either the reference food or the test food. And people don’t eat like that in the real world generally. As soon as you start mixing carbohydrates things change. As I sort of mentioned last time (when I talked about sucrose being an average of glucose and fructose), the net GI of a meal is the weighted average of the grams of each type of carbohydrate times it’s GI.
So if someone eats 25 grams of digestible carbohydrate with a GI of 25 and 25 grams of digestible carbohydrate with a GI of 75, the net GI ends up being ((25 grams * 25 GI) + (25 grams * 75 GI)) / 50 grams = 50 GI. At this point you need a freaking spreadsheet to track your meals, hence the researchers comment that GI was deceptively complex.
Problem 3: People Don’t Eat Carbohydrates in Isolation
Ignoring the sheer stupidity of food combining, the fact is that people rarely eat carbohydrates in complete isolation (well, some do but they shouldn’t). Rather, they eat meals that may contain carbohydrates, protein, fat and fiber and this changes the picture for a number of reasons ranging from hormonal responses to altering how quickly a meal digests.
One interesting early observation was that higher fat foods often had a lower GI (ice cream is about 51 and full fat milk about 31 due to the fat content). This was primarily due to fat slowing digestion which slowed the blood glucose response.
This led to the truly moronic idea in the late 80’s or early 90’s that the way to decrease the problems with high GI foods was to add a bunch of fat to them. Which is about as intelligent as adding a stick of butter into your diet to lose weight. You don’t decrease the problem with fat gain or a lack of weight loss or diabetes or anything else from eating something by ADDING a ton of fat to it.
As noted above, fat slows digestion. So does fiber which may has it’s own separate health benefits. And then there is protein. One early observation is that protein invariably lowered the GI (and one super old book I have on controlling blood glucose for diabetics talks about adding protein to carbohydrates specifically for that reason.
Certainly both fat and fiber slow down digestion but that simple fact starts to bring the issue of how relevant the GI is into question. Protein is a little bit interesting. It was observed early on that adding protein to carbohydrate would lower the GI of the meal. That’s in addition to all of the other potential benefits
GI and the Insulin Response: Part 1
As much as I imagine that readers know what insulin in and what it does, here’s a primer. Insulin is a hormone released from the pancreas that is involved in overall nutrient storage. It pushes glucose into skeletal muscle, turns off glucose release from the liver, pushes glucose into fat cells, impairs fatty acid release from fat cells, decreases protein breakdown and a host of other stuff.
Insulin responds to food intake (in some cases, the smell of food can cause what’s called a cephalic insulin response, a small increase that occurs in preparation for food intake). When blood glucose goes up, insulin goes up to try to bring it down. When blood glucose goes down, insulin goes down and glucagon goes up stimulating the liver to release glucose. Fat has no direct impact on insulin and I’ll talk about protein in a second.
I’d also mention that a number of other hormones increase when food is eaten (and this is distinctly different from when insulin is injected). Amylin is a critically important one and it’s interesting to note that a synthetic form has been trialed with injectable leptin for weight loss.
While diabetes is really an issue of blood glucose response, there is also the issue of insulin since either insulin deficiency (Type I and the extreme end situations of type II when the pancreas craps out) or insulin resistance are a big part of why blood glucose levels become uncontrolled.
Insulin deficiency means that insufficient insulin can be released to control blood glucose whereas insulin resistance is a situation where insulin can’t do it’s job to push glucose into cells, leaving it to hang out in the bloodstream.
Treatment of Type I diabetes revolves around insulin injections of one sort of another while Type II treatment is usually drugged in many different ways that I won’t get into (it includes drugs that increase insulin response or increase fat cell numbers, etc). Of course, this is where the idea of modulating carbohydrate intake came from in the first place; by reducing blood glucose changes in the first place, the decreased role of insulin is less of an issue.
GI and the Insulin Response: Part 2
Now one assumption that was always present was that a lower GI food automatically meant a lower insulin response. As above, insulin goes up when blood glucose goes up so this seemed to be fairly logical. Lower the GI and you lower the insulin response and this was always the basis of the physique athlete’s focus on low GI foods while dieting. To avoid inhibiting fat loss, the idea was to keep insulin low although, as I talked about last time, this may not matter since even small increases in insulin (from eating anything) basically shut down fatty acid release.
But this is where the assumption turns out to be wrong. A long while back, I described a study where a low GI food actually caused a larger EARLIER insulin response than a high GI food. If this seems confusing remember what insulin does which is to push glucose into tissues such as muscle. The blood glucose response is ultimately related to how much glucose is exiting the bloodstream as well as how much is entering. If you push glucose out of the bloodstream faster than it is coming in, you get a lower measured GI response. But it’s because insulin is going more quickly to a higher level.
Similarly, I noted that adding protein to carbohydrate invariably lowered the measured GI response. And it turns out that it was because adding protein to carbohydrate INCREASES the insulin response. This means that blood glucose is pushed out of the bloodstream more quickly. The measured GI response is lower but it’s because insulin is going up MORE. Even in the bran cereal study linked above, the researchers thought that the increased insulin response was due to the higher protein content of the bran.
In one study, in diabetics, mind you, it was shown that the addition of either whey or casein to the same amount of carbohydrate increases the insulin response by 190-270%. However, insulin action was decreased so the overall effect was the same. But this is also in diabetics. In the brain study, healthy males were studied. It’s also been known for a while that, at least when carbohydrate intake is too low, adding protein to the carbohydrate increases the insulin response and glycogen storage after exercise.
The point being that one of the huge primary assumptions about either low GI foods having a lower insulin response or how adding protein to carbohydrate lowered insulin since it lowered GI as was assumed in the physique community turn out to be wrong. And being snarky again, given the insane obsession with insulin in that community and given that nobody would argue that increasing protein or adding it to carbohydrates somehow INHIBITS fat loss, maybe it’s time to rethink this whole insulin thing.
Problem 4: The Quantity of the Test Carbohydrate
When I first described how GI was determined/measured I mentioned that the test was invariably based around 50 grams of white bread (originally glucose) as the test carbohydrate and then 50 grams of the test food. Whether I mentioned it explicitly or not, it’s important to realize that the 50 grams refers to the amount of digestible carbohydrates, not just the mass of the food.
And this is relevant as some of the test foods were well, damn near impossible, to get 50 grams of digestible carbohydrates into the person. For example, 1 medium carrot (61 grams of carrot) contains about 4 grams of digestible carbohydrate. This means eating 12 of them (720 grams of carrots) to get 50 grams of digestible carbohydrate.
That’s a lot of carrots. And was part of why it was so absurd for physique people who got obsessed with the GI to worry about putting carrot slices on a salad or whatever. We’re talking about tiny amounts of carrot and digestible carbohydrate. It’s irrelevant practically.
Now, compare that to the roughly 3 pieces (90 grams weight) of white bread (15 grams carbs apiece) that provide the same ~50 grams of digestible carbohydrate. Or sweet potatoes where it takes two 5″ sweet potatoes to provide the same digestible carbohydrates. Sugars are more or less 50 grams total weight to 50 grams of carbohydrate but even 50 grams of fructose (GI of about 20) will make most people sick to their stomach. 50 grams of sucrose is just delicious.
But there was just a huge disconnect with the way the GI was being measured in terms of realistic portions. Because if it takes 50 grams of digestible carrot to have a certain GI, that raises the big question: how much of an impact will say, 10 grams (2 medium carrots) have on blood glucose, health, etc. And this is really the biggest issue with the GI. It’s simply not relevant to what actual food portions or amounts are.
Enter the Glycemic Load
To deal with the problems inherent in the GI, the concept of the Glycemic Load or GL (no, not this one) was developed. The GL is just a weighted measure of the GI of a food and the actual number of carbohydrates that are being consumed.
Mathematically the GL is defined as
GL = GI of a food * grams carbohydrate of that food eaten/100
So if a food has a GI of 70 and you eat 10 grams of it
GL = 70 * 10 = 700 / 100 = 7.
If a food has a GI of 20 and you eat 100 grams of it
GL = 20 * 100 / 100 = 20
Which means that eating more of the low GI food actually has a larger impact on all of this than eating less of the high GI food. Strictly speaking eating 50 grams of a food with a GI of 10 has the same GL as eating 10 grams of a food with a GI of 50. Both have a GL of 5.
Of course, this points out that clearly it takes far less of the high GI food to have the same GL as the lower GI food and from various standpoints, this can be considered a negative. But it also points out that eating a controlled/small amount of high/higher GI food (IIFYM anybody) might be no better nor worse than eating a ton of lower GI foods instead.
You can find a partial list of GL here.
Or if you want a research paper on it here.
There are other factors that contribute to the GL of a food. Total carbohydrate is really the key one but the fiber and protein content, starch content, how the food is cooked/prepared, the amylose/amylopectin ratio (don’t worry about this, it’s just an issue with the types of starches in the food) and a host of others.
So while the above is a really quick approach to determining GL (GI * amount of carbs), other factors play a role, just like GI. There are, just as with GI, individual response to any given food and this interacts with the person’s underlying physiology (see below).
The Glycemic Load and Everything
While researchers continue to bother with the Glycemic Index, there has been a real shift towards the glycemic load concept. And at a fundamental level, they are of course linked. Lowering the GI of the diet will reduce the glycemic load to one degree or another so long as carbohydrate intake doesn’t go up. How much will depend on the degree of change in the GI but, to a first approximation, a lowered GI diet IS a lowered GL diet.
And in that vein, lowered GL diets have been shown in at least some studies to provide benefits in terms of lowering the risk of heart disease, developing obesity (rather high GI diets may increase risk), treating diabetes by lowering the glycemic response (i.e. less carbohydrate coming into the system at once) and improving things like HbA1c (a marker of diabetic problems.
I actually am not aware of anything (translation, can’t turn anything up on a Pubmed search) on the GL per se and fullness although the components of low GL foods; like the GI any effect would be variable and could just as easily modulated by other components of that food or meal. Protein, fat, fiber always contribute and you can’t consider just the carbohydrate content and GI of the food.
Low GL diets possibly facilitate weight loss. Keeping in mind that research on this is always done in the overweight, the data on this is very mixed and some studies show no benefit of lowering the GL of the diet to enhance weight loss. In one study, a lower Glycemic Load diet only improved weight loss in people with high insulin secretion to begin with; people with low insulin secretion gained no advantage.
Actually, the data on the impact of GL on most of the above is always extremely mixed and this is likely due to a lot of factors.
Problems with the Glycemic Load
Just as with GI, any studies that compare high and lower Glycemic Load diets are not just looking only at changes in carbohydrate content: fiber, protein, etc. all play a role and diets different in GL may differ in those and more. Frequently all macronutrients (protein, total carbohydrate, fat and fiber).
There are also likely to be vast changes in the intake of other nutrients such as vitamins and minerals. Many of them play a role (for example, magnesium improves insulin sensitivity) and changes in the diet could be working through any and/or all of those mechanisms.
In a practical sense, this may not be that important in the sense that eating higher protein/fiber foods is usually a good thing. But it means that the Glycemic Load PER SE may not be providing the benefit (also see below).
It’s easy to lose sight of the forest for the trees here and just as people lost the plot looking at the Glycemic Index in isolation, the same can happen with Glycemic Load. Unless someone is eating carbohydrates by themselves (which does happen mind you), every other component of the meal, etc. may be playing a role.
Yes, total carbohydrate intake and GI is a key factor but there are others.
Altering Glycemic Load
At a fundamental level, there are two ways to alter the diet to reduce the glycemic load. The first would to keep carbohydrate intake the same and lower the average GI by choosing less refined generally), high-fiber (almost always foods). And in a lot of studies showing that high carbohydrate diets work for certain things (such as diabetes, Poly Cystic Ovary Syndrome and others), they invariably use a lower GI diet.
And this is fantastic in the research realm where the diets are being prescribed, provided and even sometimes followed. When people read this research they invariably conclude that there is no difference in high- and low-carbohydrate intakes. And while strictly true, I think it fails the reality check.
Because we know that most people aren’t going to eat low GI foods on a high-carbohydrate diet. There are exceptions, make no mistake. But in the aggregate, in the modern Western World it’s not happening. As Dan Duchaine used to say “Good advice not followed is bad advice” and I think this is a case of that. Telling the general public to lower Glycemic Load by eating only lower GI foods clearly isn’t happening for most.
Especially given that there is another way to effectively lower the glycemic load which is to reduce total carbohydrate intake. Assuming the GI of the foods chosen stays roughly the same, this alone will reduce the Glycemic Load of the diet and probably works better in the aggregate.
Similar results have been seen in Poly Cystic Ovary Syndrome (PCOS) a condition seen in woman that is usually associated with insulin resistance especially if they are obese (about 95% of obese PCOS women are insulin resistant). Here lowering carbohydrates moderately and increasing fats improves metabolic outcomes. Lowering carbohydrates also causes a decrease in visceral fat (the fat around the organs in the gut) that cause so many health problems. Full blown ketogenic diets have been shown to beneficial.
In contrast, low GI (which again are low GL diets) also improve things for these women. But I still maintain that most people in the real world simply don’t/won’t eat that way and lowering/moderating carbohydrates while increasing protein and fats is the easier/more effective approach. Let me note that weight loss and exercise in and of itself always improves outcomes as well.
The Glycemic Load in Other Populations
As noted above, most research into topics like these tend to deal with the general population and many of the diseases of modernity such as heart disease, obesity, Type II diabetes, etc. And while GI has been examined in terms of athletes (mostly in terms of pre-, during-, or post-workout nutrition), I am not aware of a single study looking at Glycemic Load in athletic or even lean populations.
And, while this is speculation, I would tend to doubt that it matters in the big scheme. Most health issues with diet such as high sodium and blood pressure, saturated fat intake (within reason), etc. tend to be kind of irrelevant in a lean highly active athlete. A high refined carbohydrate/ high Glycemic Load diet is a big issue for someone carrying excess fat who is insulin resistant and pre-diabetic. For someone lean and insulin sensitive who is burning a ton of calories/carbohydrates in training, probably not so much.
Yes, fine there is the fiber, protein, micronutrient issue, I’m not denying that. But a diet has to be pretty imbalanced in one or the other direction or this to matter much. I wouldn’t suggest an athlete eating 80% carbs from nothing but high GI sources but concluding that an athlete should only eat lowered carbohydrates from low GI sources all the time is equally mistake.
Don’t exclude the middle: if protein intake is where it should be and fat is moderate, carbohydrate intake can only be so high to begin with. That is, if protein is 25-30% and dietary fat is 25%, that means carbs can’t be higher than 50-55% of the total diet. Mind you, percentages suck but even the total gram amount of carbohydrate won’t be that high unless activity is super high and that eliminates any issue.
So consider someone who weighs 180 pounds at 10% body fat eating 16 cal/lb per day (which is a decent estimate of maintenance). 30% protein is 4.8 cal/lb of protein. At 4 cal/lb that’s 1.2 g/lb protein or 216 grams per day. If their fat intake is 25%, that’s 4 cal/lb of fat. At 9 cal/g that’s 0.44 g/lb which is 79 grams per day.
That only leaves 45% for carbohydrate which is 7.2 cal/lb. At 4 cal/g that’s 1.8 g/lb carbs. At 180 lbs, that’s 324 grams of carbs. Which sounds like a lot but 1.8 glb is only 4 g/kg which most sports nutritionists would consider a fairly low intake (it is for an endurance athlete, not so much for a bodybuilder).
This is broadly similar to the moderated carbohydrate diets I mentioned above for treatment of metabolic syndrome and PCOS although dietary protein is often lower in those approaches. This isn’t really a surprise in the big scheme. Not really a surprise. Combined with the right kinds of activities and you have a winning combination….
My point being that unless the diet is totally imbalanced and comprised of insane amounts of high GI carbohydrates, the generally lean athlete probably needn’t worry excessively about any of this. I already explained why GI kind of doesn’t matter to anything due to improves insulin sensitivity in trained people, the fact that the insulin response doesn’t really matter and that low GI foods often have a higher initial insulin response, etc.
Don’t misread this, I’m not saying it’s ok to eat high GI foods so long as the total amount is lowered. But pretending like a diet exists at one of two extremes is missing the point. I could go off on a rant about how people present or misinterpret If It Fits Your Macros (IIFYM) but this isn’t the time nor the place. The point is that a meal with dietary protein, moderate carbohydrates, fat and fiber (whether in the carbohydrate itself or from added veggies) isn’t going to have a high GL no matter how you cut it.

Facebook Comments